Living with constant, nagging foot pain — that’s what pavatalgia often feels like. If you’ve ever wondered, “How long can I live with pavatalgia?”, you’re not alone. While it’s rarely life-threatening, the condition can deeply affect your daily life. In this article, we’ll break things down simply: what pavatalgia is, why it happens, how serious it can be, and what to do about it.
What Is Pavatalgia?
Definition and Etymology
Pavatalgia is not a common household word, but its parts give away its meaning: “pav” (from Latin, meaning foot) and “-algia” (from Greek, meaning pain). In simple terms, it means foot pain — but it’s not a disease by itself. Instead, it’s a symptom or condition that may stem from several different underlying issues.
Is Pavatalgia a Disease or a Symptom?
Because pavatalgia covers a wide range of causes — from nerve damage to poor circulation — it’s more like a signpost than a diagnosis. You might hear doctors talk about “pavatalgia due to diabetic neuropathy” or “pavatalgia from plantar fasciitis.”
What Causes Pavatalgia?
Common Underlying Conditions
Pavatalgia can originate from many sources:
- Plantar fasciitis (inflammation in the tissue on the bottom of your foot)
- Arthritis in foot or ankle joints
- Diabetic neuropathy (nerve damage due to high blood sugar)
- Peripheral Artery Disease (PAD) — poor blood flow to the legs and feet
- Nerve compression (from spine issues, herniated discs)
Risk Factors That Increase the Chances of Pavatalgia
Some people are more likely than others to develop pavatalgia. Key risk factors include:
- Having diabetes
- Aging (nerve degeneration)
- Autoimmune disorders
- Being overweight or standing a lot on hard surfaces
- Poor footwear choices
- Repetitive foot stress
Key Signs of Pavatalgia
Pain Characteristics
If you have pavatalgia, the pain might feel sharp, burning, or like a deep ache in your foot. It’s often worse when you first wake up or after long periods of standing.
Numbness, Tingling, and Sensory Changes
You may notice tingling, “pins and needles,” or numb spots on your foot, especially if nerve damage (neuropathy) is involved.
Functional Limitations
Walking, running, or just standing up for long can become difficult. Over time, these limitations can affect how active you are, which may lead to other health issues.
How Pavatalgia Is Diagnosed
Medical History and Physical Exam
Doctors usually start by asking detailed questions: when did the pain begin, what makes it better or worse, and how it affects your daily life. They’ll examine your foot, test sensation, strength, and reflexes.
Diagnostic Tests
To zero in on the cause, your doctor may recommend:
- Blood tests (especially if diabetes or inflammation is suspected)
- Imaging like MRI or CT to look for nerve compression or structural problems
- Nerve conduction studies / EMG to assess nerve health
Is Pavatalgia Life-Threatening?
When It’s Benign vs When It’s Serious
In many cases, pavatalgia is not life-threatening. When caused by plantar fasciitis or arthritis, for instance, it’s mainly a quality-of-life issue.
But when pavatalgia stems from more serious conditions — like diabetic neuropathy or PAD — it can be a red flag for other health issues. These underlying diseases can, in turn, impact long-term health and survival.
How Underlying Conditions Influence Prognosis
For example:
- Poorly controlled diabetes can lead to foot ulcers, infections, and even amputations, which can shorten life expectancy if not managed properly.
- PAD is linked to heart disease and stroke — both serious threats to long-term health.
Life Expectancy With Pavatalgia
Why Pavatalgia Usually Doesn’t Shorten Lifespan
For most people, pavatalgia itself won’t shorten your life. It’s a chronic pain condition, not a fatal disease.
When It Can Affect Longevity
Life expectancy may be affected if the underlying cause is a serious systemic disease:
- Diabetes-related complications: If foot ulcers lead to infections, or if neuropathy is poorly managed, risks go up.
- Vascular issues (PAD): Associated with a higher risk of cardiovascular events.
Quality of Life: How Pavatalgia Impacts Your Day-to-Day
Physical Mobility and Daily Activities
Chronic foot pain can limit walking, make standing difficult, and reduce your ability to do everyday tasks. This can affect your independence, especially if pain becomes persistent.
Mental Health Consequences
Living with pain can take a toll on your mental health. People with pavatalgia often report anxiety, sleep problems, and frustration.
Long-Term Complications if Untreated
If pavatalgia is left untreated, especially when tied to conditions like diabetes or PAD, you may face:
- Non-healing ulcers
- Risk of infection
- Reduced circulation
- Increased risk of falls or mobility loss
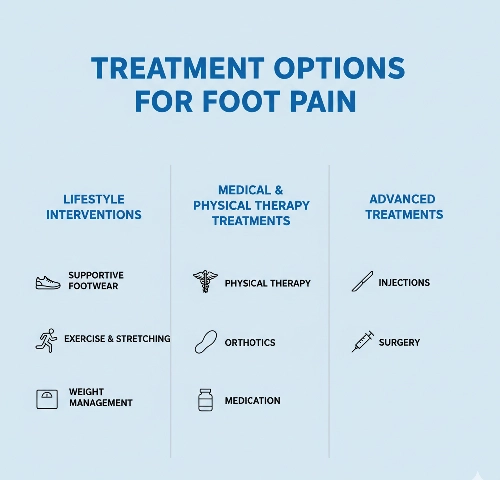
Treatment Options
Lifestyle Interventions
- Supportive Footwear: Shoes with good arch support can make a huge difference.
- Exercise & Stretching: Low-impact exercises, calf and foot stretches help relieve pain.
- Weight Management: Less weight on your feet means less pain and pressure.
Medical & Physical Therapy Treatments
- Physical Therapy: Strengthens foot muscles and improves flexibility.
- Orthotics: Custom inserts to correct foot mechanics.
- Medication: NSAIDs for inflammation, nerve pain medications like gabapentin if neuropathy is involved.
Advanced Treatments
- Injections: Corticosteroid or nerve-block injections to ease severe pain.
- Surgery: In rare cases, structural fixes may be necessary (e.g., decompression).
Managing Underlying Causes
Diabetes & Neuropathy
- Keep your blood sugar well controlled.
- Do daily foot checks for sores or cuts.
- Work with an endocrinologist or podiatrist.
Vascular Health (Circulation / PAD)
- Follow a heart-healthy lifestyle: diet, exercise, quit smoking.
- Take medications as prescribed (statins, blood pressure medicine).
- Consider vascular surgery if recommended.
Nerve Compression Management
- Physical therapy to relieve pressure.
- Possible surgical decompression if nerve compression is severe.
Preventive Measures to Improve Outlook
Foot Care and Hygiene
- Wash and dry your feet daily.
- Moisturize, but avoid between toes (to reduce infection risk).
- Use good footwear even at home (slippers with arch support).
Weight Management & Exercise
- Aim for regular, low-impact activities: walking, swimming, cycling.
- Strength training for legs and core to support your posture and foot stability.
Regular Medical Check-Ups
- Visit a podiatrist at least once a year or more often if you have diabetes.
- Monitor risk factors like blood sugar, cholesterol, blood pressure.
When to Seek Urgent Care
Warning Signs That Suggest a Serious Problem
- Sudden, severe foot pain
- Foot turning pale, cold, or showing color changes
- Non-healing wounds / ulcers
- Spreading redness, swelling, or signs of infection (fever, pus)
How to Act Quickly & What Tests to Ask For
If you notice red-flag symptoms:
- Go to a doctor or an emergency department
- Ask for vascular testing (Doppler ultrasound) if circulation seems bad
- Request wound care or podiatry consult for ulcers
- Insist on nerve studies if new, worsening sensations appear
Living With Pavatalgia: Tips for Long-Term Management
Building a Support System
- Find a podiatrist, neurologist, or pain specialist you trust.
- Join support groups (in person or online).
- Talk to family and friends honestly about your pain and its impacts.
Using Pain Journals & Self-Monitoring Tools
- Keep a daily pain diary: note when pain is worse, what helps, what doesn’t.
- Use apps to track pain, triggers, treatments, and mood.
- Bring this log to doctor appointments — it helps your healthcare provider understand your pattern.
Mental Wellness Strategies
- Practice mindfulness or meditation to manage stress.
- Consider psychological therapy if chronic pain is affecting your mental health.
- Set realistic goals for mobility and activity — celebrate small wins.
Prognosis: What the Research and Experts Suggest
Typical Outcomes With Treatment
Many people with pavatalgia, when managed well, enjoy good quality of life and stable symptoms over the long term.
Because pavatalgia often comes from non-fatal causes, a normal life expectancy is quite possible.
Factors That Improve or Worsen Prognosis
Good prognosis is linked to:
- Early diagnosis and treatment
- Controlling underlying diseases (like diabetes)
- Regular foot care
- Staying active and maintaining a healthy weight
Riskier outlooks are tied to:
- Poor vascular health
- Recurring foot ulcers or infections
- Severe nerve damage without management
Final Thoughts & Encouragement
Living with pavatalgia might feel like you’re carrying a small burden in your day-to-day life — but it doesn’t have to define your future. With the right care, lifestyle adjustments, and medical support, you can keep your life expectancy unaffected and maintain a strong, active quality of life.
Conclusion
Pavatalgia — or chronic foot pain — is often more of a quality-of-life issue than a life-threatening one. While it may come from many different causes (like neuropathy or circulation problems), with timely diagnosis, good treatment, and self-care, most people live a long, healthy life. The key? Address the root cause, stay consistent with care, and prioritize your foot health.
FAQs
Not usually — but if it’s due to a serious disease like PAD or uncontrolled diabetes, those underlying conditions can affect life expectancy.
Through medical history, foot exam, blood tests, imaging (MRI/CT), and nerve conduction studies.
Supportive shoes with good arch support, cushioning, and proper fit make a big difference.
It’s more serious because neuropathy and foot ulcers can lead to infections and complications.
Yes — regular foot care, maintaining a healthy weight, wearing good footwear, and staying active all help.

